In many Indian villages, getting medical care still means borrowing money, missing work, or walking miles to the nearest clinic. A fever often goes untreated. A diabetic patient waits until the symptoms get worse. And for someone managing high blood pressure, regular monitoring is more a hope than a habit. The burden isn’t just medical — it’s social, economic, and deeply personal.
Despite numerous efforts and policies aimed at strengthening rural health, long travel times, limited doctor availability, and lack of diagnostic services make quality healthcare feel distant and unreliable. A 2023 study found that more than 60% of rural Indians travel outside their state for medical treatment due to the poor availability of local healthcare services. This often leads to late diagnosis, worsening of chronic conditions, and additional financial burdens on already stretched households.
But this story is starting to change. Remote care, including telemedicine and digital health platforms, is beginning to bridge the gap. India’s free-to-use National Telemedicine Service, eSanjeevani, has provided over 276 million consultations and shown promise to reduce systemic inequalities in access to care. These services are allowing villagers to consult doctors from home, get prescriptions digitally, and even have their vital signs monitored remotely using simple medical devices.
In the sections ahead, we explore how remote care is making a social difference, not just a clinical one — improving lives by cutting travel costs, building trust, and empowering families to take charge of their health.
The Rural Healthcare Landscape
Before we dive into the social impact of remote care, let us analyze the current scenario. India’s healthcare infrastructure is heavily skewed towards urban areas. Approximately 75% of health resources are concentrated in cities, serving only 27% of the population. This disparity leaves rural communities with limited access to medical professionals and facilities. For instance, as of March 2023, India had 1,69,615 Sub-Centers (SCs), 31,882 Primary Health Centers (PHCs), 6,359 Community Health Centers (CHCs), 1,340 Sub-Divisional/District Hospitals (SDHs), 714 District Hospitals (DHs), and 362 Medical Colleges (MCs) serving both rural and urban areas, according to the Ministry of Health and Family Welfare. Despite these numbers, many rural residents travel over 100 km to access healthcare facilities.
The Emergence of Remote Care
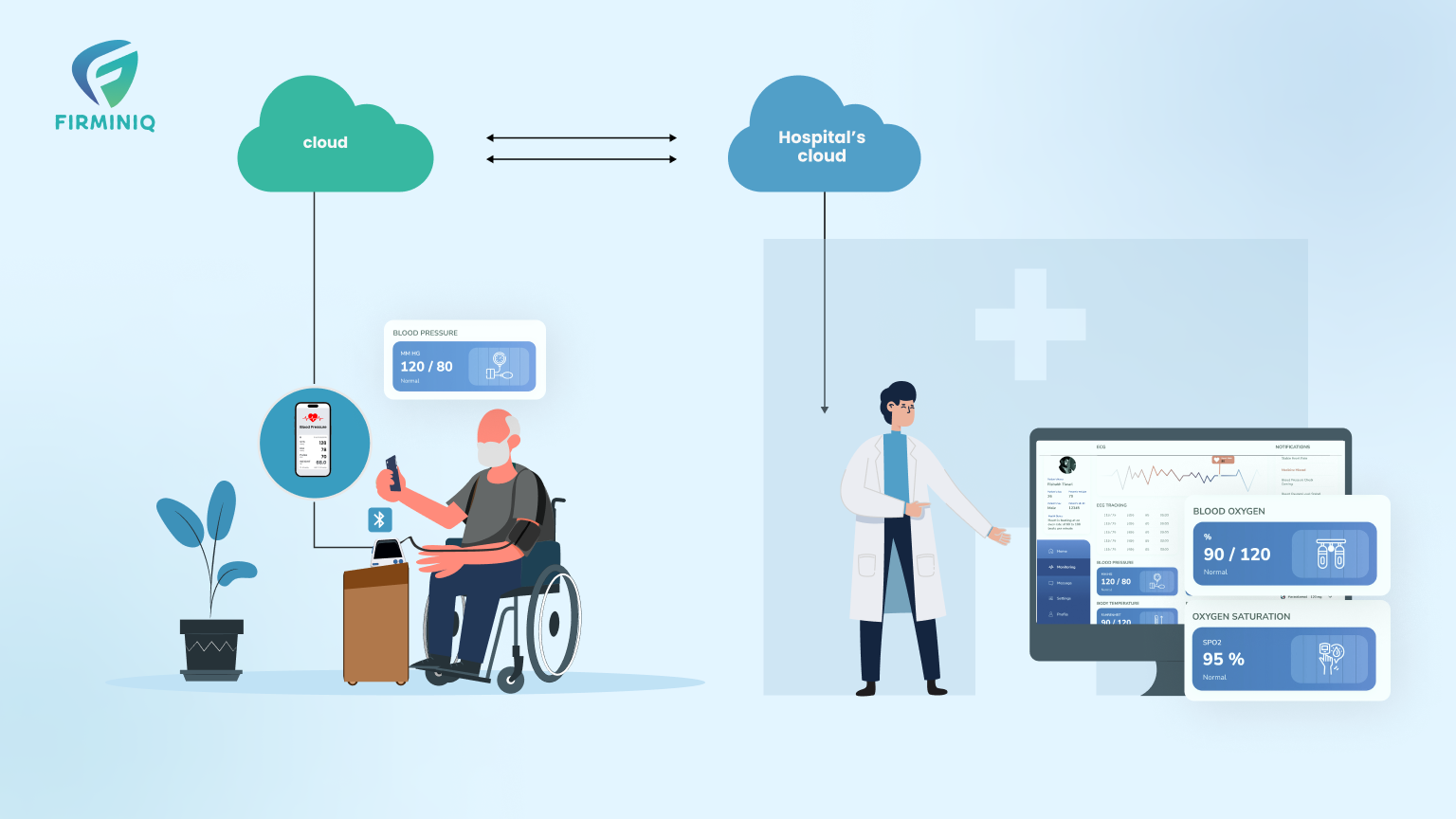
Remote care is steadily becoming a lifeline in rural India. With the help of mobile phones, simple health monitoring devices, and improving internet access, people in villages can now consult doctors without needing to travel long distances. From getting advice on common illnesses to managing chronic conditions like diabetes or high blood pressure, patients are receiving timely support from the comfort of their homes. These digital interactions help families feel more in control of their health and are reducing the stress and costs that come with traditional care. As awareness and usage grow, remote care is quietly reshaping how healthcare reaches those who were once left out.
Social Impact of Remote Care
Here’s how remote care is making a tangible social difference in rural India:
Cutting Travel Costs and Time
In rural India, accessing healthcare often entails traveling long distances to reach medical facilities, leading to significant expenses and time loss. Telemedicine has emerged as a solution, enabling patients to consult with doctors remotely, thereby reducing the need for travel.
Building Trust in Healthcare Systems
Telemedicine platforms have played a pivotal role in building trust among rural populations by providing consistent and reliable healthcare services. The eSanjeevani platform, for example, has been instrumental in delivering quality consultations, with a significant number of patients returning for follow-up sessions, indicating growing confidence in digital healthcare solutions.
Enhancing Continuity of Care
Remote care ensures continuous monitoring and follow-up, especially crucial for managing chronic conditions. Telemedicine allows for regular check-ins and timely interventions, reducing the risk of complications and hospitalizations.
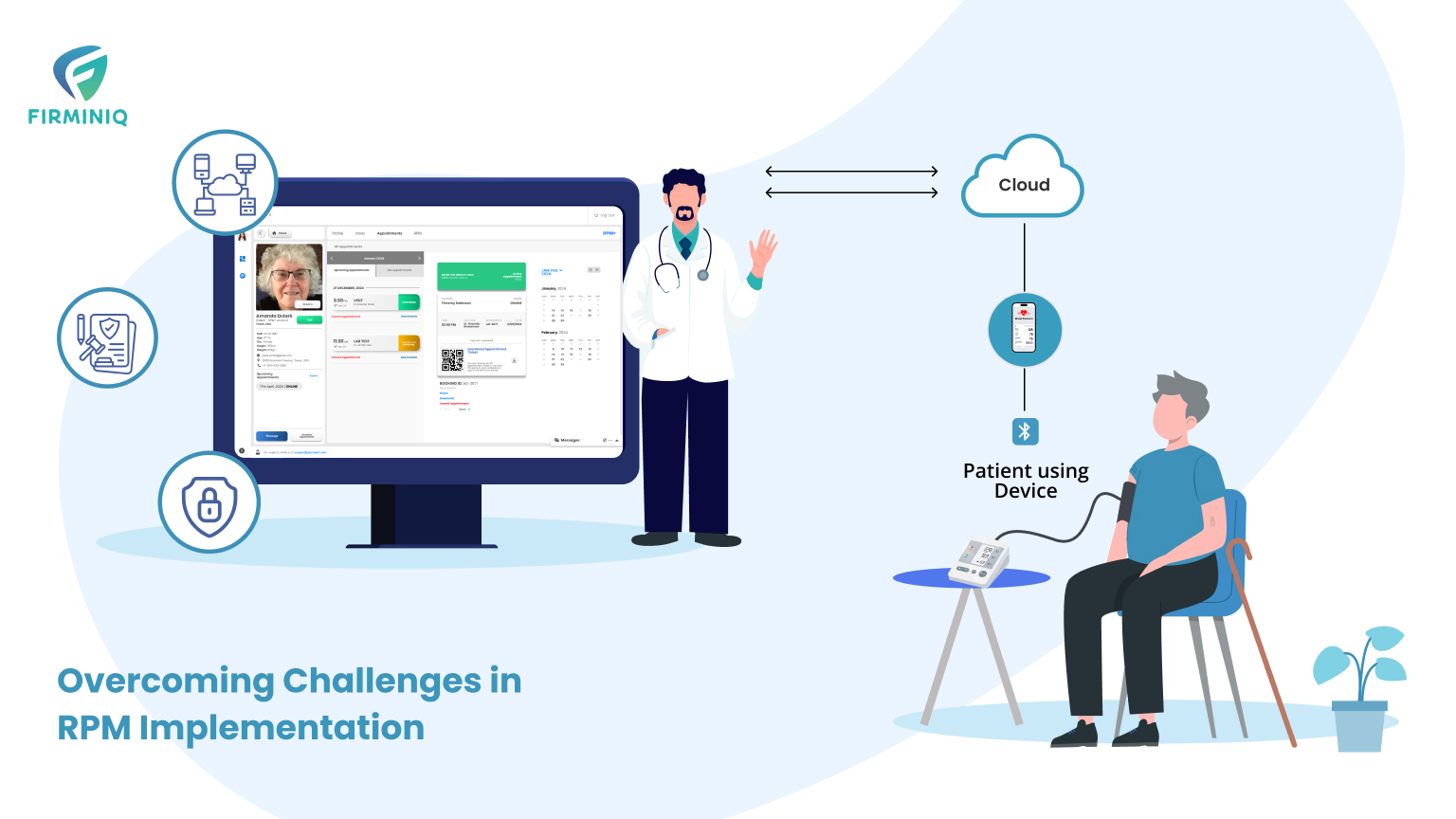
Addressing Infrastructure and Literacy Challenges
While telemedicine offers numerous benefits, challenges like limited internet connectivity and digital literacy persist. Programs like the Common Service Centres (CSCs) under the Digital India initiative aim to bridge this gap by promoting digital literacy among rural citizens, thereby facilitating the adoption of telehealth services.
Scaling the Change Further
While remote care is gaining ground, scaling it across India’s vast rural expanse requires deeper coordination:
- Local Language and Low-Tech Support: Audio-first interfaces, dialect options, and offline consultation features will help make remote care truly universal.
- Incentivizing Rural Doctors: Providing incentives and support for doctors serving rural patients via telehealth can help address professional shortages without requiring relocation.
- Expanding Beyond Primary Care: RPM and telehealth can be used for chronic care programs, geriatric support, mental health, maternal care, and lifestyle coaching.
Conclusion
Remote care is not just a technological advancement; it’s a new approach to making healthcare more accessible. By reducing travel burdens, building trust, educating families, ensuring continuity of care, and addressing infrastructural challenges, telemedicine is reshaping the healthcare landscape for the better.
Platforms that go beyond just treatment and focus on connection, education, and prevention will define the future of rural healthcare. If you are looking to build one, get in touch today!